
It might seem that we do not use our pelvic floor muscles in everyday life . Nothing could be further from the truth. This structure plays a very important role. Pelvic floor muscle exercises are not difficult and can produce impressive results - and in a short time. With regular gymnastics, their function improves, and thus unpleasant discomforts subside.
Take back control of your sensitive bladder! Physical therapy is one of the best ways. The easiest type of therapy is pelvic floor exercise plan, which strengthen your pelvic floor and help treat both stress incontinence and urge incontinence. So let us help you how do to pelvic floor exercises for women – read on for more!
Many women – in fact, 1 in 3 – experience some form of urinary incontinence. Strengthening your pelvic floor muscles can greatly increase your ability to avoid little leaks throughout the day. Pelvic floor exercises for women can help you regain control of your bladder, your life and your self-esteem, making those little leaks more manageable.
Table of content:
- What are pelvic floor muscles?
- How to do pelvic floor exercises step by step?
- Pelvic floor exercises plan
- Making pelvic floor exercises routine
- Additional exercises that strengthen your pelvic floor muscles
- Pelvic floor exercises in pregnancy
- Pelvic floor exercises after childbirth
- Other methods for improving bladder control
What are pelvic floor muscles?
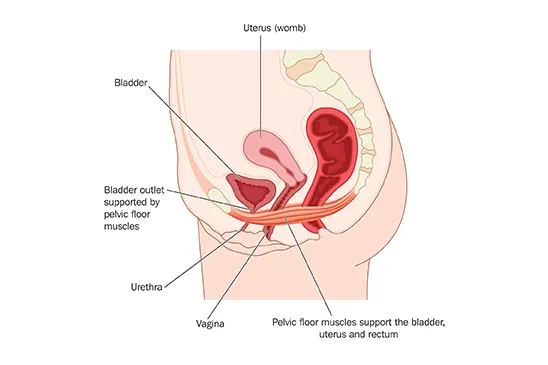
The pelvic floor is a system of muscles, ligaments, tissue, and nerves arranged at the bottom of the pelvis that form a hammock supporting your bladder and uterus. The pelvic floor muscles female are actually made up of several different muscles. These are:
- the anal lever muscle,
- external anal sphincter muscle,
- urethral sphincter muscle,
- cusp muscle,
- superficial transverse perineal muscle,
- deep transverse perineal muscle,
- ischio-cavernosus muscle.
This structure has a second name - the Kegel muscles. It is widely used. It comes from the name of a doctor who, as early as the middle of the last century, actively promoted training on the pelvic floor muscles, described its benefits and proposed a set of exercises.
The Kegel muscles extend all the way from the bottom of the abdomen to the buttocks. It is a very extensive and complex structure. It also has good innervation.
The muscles of the pelvic floor extend from the pubic symphysis to the anus. They surround the urethra, rectum, bladder outlet and fill the genital area. The pelvic floor muscles can be easily felt. The easiest way to do this is on the toilet. All you need to do is suddenly stop the stream of urine. This test should be done once. The structures that tighten at this point are the Kegel muscles.
As women, our pelvic floor goes through a lot, especially during pregnancy and childbirth. In fact, natural childbirth and C-sections can increase your chances of developing urinary incontinence after having children. Exercising your pelvic floor muscles helps to prevent and manage incontinence and can make sex more pleasurable.
Pelvic floor exercises are easy, and you can do them anytime, anywhere. Just follow this simple how–to guide to start strengthening your pelvic floor muscles right now!
How to do pelvic floor exercises step by step?
Pelvic floor muscle exercises have many benefits for the body. First and foremost, they improve the blood supply to the tissues in the lower abdomen. This structure not only becomes stronger, but also more elastic. At the same time, the functioning of all other organs that are surrounded by the Kegel muscles improves.
Training is one of the methods of treatment and prevention of stress urinary incontinence. This condition is very common. It occurs as a result of weakened pelvic floor muscles. To make pelvic floor exercises for women more effective more quickly, it is also worth remembering to strengthen the whole body. The muscles of the abdomen, thighs and buttocks deserve special attention.
How to do pelvic floor exercises? You can start toning your pelvic muscles as you read. Just follow these simple steps:
- Squeeze the muscles that you use to stop your urine flow. Make sure that you focus on only your pelvic muscles. Now pretend your vagina is a lift and you are going upwards. Be careful not to squeeze the muscles of the leg, buttock or abdomen instead.
- Hold for at least 4 seconds. The more often you do this, the “higher” you can go. Try holding for up to 10 seconds.
- Slowly exhale through your mouth and gradually release the hold. Repeat 10–20 times in a row at least 3 times a day.
- You can test your pelvic floor muscles with a simple stop–start test. When going to the toilet, begin to urinate and cut off the flow by contracting the muscles. If you experience better control than before, you know the pelvic floor exercises are working.
Pelvic floor exercises plan
To maximise the benefits of your pelvic floor workout, exercise the muscles with both long and short squeezes, repeating until the muscles feel tired. It is also important that relaxing the muscles takes the same amount of time as tensing them - for example, when tensing the muscles you count to 3 and when relaxing them you should also count to 3.
There are two types of exercises:
- LONG SQUEEZES Tighten your pelvic floor muscles and hold for several seconds and then relax for the same length of time. Start with 5 seconds and work your way up to 10 seconds as you get practice.
- SHORT SQUEEZES Tighten your pelvic floor muscles for one second, then relax.
Remember never to exercise while urinating, as this can disrupt urinary function. The first effects of the exercises should be visible after about six weeks. However, this does not mean that you have to stop doing them after this time. It is advisable to continue but, for example, with less frequency. If, despite the training and application of the above recommendations, no effect is seen, it is worth consulting a urogynaecological physiotherapist.
Making pelvic floor exercises routine
Pelvic floor exercise routine is the best way to start practising in everyday life. Here are some ideas for fitting pelvic floor exercise program into your schedule. Try to work your pelvic floor exercises into existing routines to help to make your pelvic floor stronger. That way, you can use it when you need it. When exercising, remember an important rule - focus only on your pelvic floor muscles, do not tighten your abdominal muscles, buttocks or thighs during your workout.
- Driving. As long as your pelvic floor exercises don’t distract you from driving, flex and release on your way to the shops, as you leave the bank, or en route to any other errands you run regularly.
- Cooking. Try to focus on your pelvic floor muscles as you carry out simple, routine cooking tasks, like stirring a pot or washing up dishes.
- Watching TV. Have favourite programmes you never miss? Exercise as you view no one around you even knows you’re busy re–claiming control of your bladder!
- At work. Do you work at a desk for extended periods? Use any down time to work out those pelvic floor muscles.
- Reading. Whether it’s the morning paper or that newest novel you can’t put down, reading as you exercise helps your repetitions to fly by.
- Bedtime. As you wind down each night, finish your last set of pelvic floor exercises before drifting off to sleep. If you keep at it, the nightmares of bed pads may be a thing of the past.
Additional exercises that strengthen your pelvic floor muscles
Pelvic floor workout described above are the simplest and most common way to help strengthen your pelvic floor muscles female. However, you can complement these exercises with other suggestions that may also help you if you have a problem with incontinence. Although you may not feel it, your pelvic floor is activated in conjunction with other muscles when performing certain movements, and not just during exercises that specifically target the pelvic floor. Here are a few pelvic floor exercises step by step exercises that help to strengthen those important little muscles with body weight. They don’t require any equipment and are easy to do in the comfort of your home.
Pelvic floor exercise step by step: Squats
- Keep your feet hip width apart, on slightly bent knees
- Engage your ab muscles (and tighten your pelvic floor, too!)
- Keeping your lower back braced, lower your body into a squat
- To avoid injury, make sure your knees stay in line with your toes
- Rise back up to standing position, do not fully straighten the knees
- Repeat

Pelvic floor exercise step by step: Bridges
- Lie on the floor
- Bend your knees and place your feet firmly on the floor, keeping your knees in line with your hips, feet should be positioned at hip width
- Tighten your pelvic floor muscles and push your hips up off the floor, keeping your back straight
- Hold this position for 10 seconds
- Relax, you can put your hips back on the ground or leave them in the air
- Repeat

Pelvic floor exercise step by step: Bird dogs
- Start on all fours, making sure to keep your wrists aligned under your shoulders, and your knees under your hips
- Keep your head facing down so your spine is in alignment, don't lift your head up
- Tighten your abs, lower back, and pelvic floor muscles
- Simultaneously raise your right arm and left leg until they are straight. Do not raise your head. Hold this position for 5 seconds
- Lower your arm and leg back to the starting position while maintaining stability.
- Perform the same movement, but with your left arm and right leg. Hold for five seconds
- Repeat 5 times on each side

What’s next?
Once you’ve learned how to do pelvic floor exercises, after 4–6 weeks of working out your pelvic floor muscles regularly, you may start to notice an improvement in your urinary incontinence symptoms.
If you’ve made a habit of pelvic floor exercises and don’t notice an improvement in your sensitive bladder symptoms, it’s time to talk to your doctor. They may recommend combining pelvic floor exercises with other treatments like sensitive bladder training or other medications, devices or procedures to help you to manage your incontinence.
Check also how to reduce urinating at night.
Pelvic floor exercises in pregnancy
Adequate pelvic floor exercises in pregnancy help to strengthen muscles that are under great strain during pregnancy and childbirth. Every woman should do pelvic floor exercises in pregnancy, regardless of her age, as this will reduce or avoid [stress urinary incontinence](/en-gb/incontinence-advice/bladder-problems/what-is-stress-incontinence-symptoms-causes-and-treatment). The first thing to start with is kegel exercises pregnancy. Kegels are the most popular exercises for the pelvic floor muscles and are fundamental if you want to strengthen them. Anyone can do them, and they are especially recommended during pregnancy. It is important to involve the pelvic floor muscles when doing them, but also the abdominal muscles.
To start exercising your kegel muscles, start by feeling them. This can be done in any position - lying down, sitting or standing. To squeeze them, make a movement as if you were trying to cut off the flow of urine. If you can't feel them, you need more practice or you may have over-tight or weak muscles.
It is also important to engage the lower abdominal muscles during exercise. This involves pushing your abdomen inwards, as if you were pulling your belly in. Do these exercises quickly at first and then hold the squeezes for as long as you can (you can count to 10). Do 3 series of 8 squeezes each day.
In addition, practise tensing your pelvic floor muscles when you cough and sneeze and remember to stretch gently to relieve muscle tension.
Pelvic floor exercises after childbirth
After giving birth, your body needs time to recover. If your muscles are weak, you may have stress urinary incontinence after pregnancy. You can relieve this by doing pelvic floor exercises after childbirth, which will allow faster recovery. Post-pregnancy pelvic floor training can be started within 24 hours of delivery, even having stitches after a perineal incision.
After consulting your doctor, you can try to return to exercising your kegel muscles. You can also start with the more comfortable pelvic floor exercises after childbirth. You can try the following exercise:
- lie down and bend your legs,
- squeeze the muscles around your back and tighten them, as if you were trying to stop urination,
- take a breath in and tighten your muscles,
- lift your bottom up (keep your shoulders on the floor)
- then when you exhale, relax and return to the original position.
If you haven't done these exercises before then do them quickly at first and then increase the time.
You can also perform another exercise in this position. With your legs bent, lower one to the side, making sure there is no rotation of the pelvis. Then bring the leg back to the centre and repeat this movement for the other leg.
If you feel that this is insufficient then ask your doctor for a referral for physiotherapy.
Other methods for improving bladder control
How to improve bladder health? There are many solutions, but whatever treatment or remedy you choose, you need to exercise your bladder and pelvic floor muscles.
- Biofeedback - If you’ve tried and have trouble doing pelvic floor exercise routine, you may want to see a physiotherapist who specialises in women’s pelvic health. A physiotherapist may suggest biofeedback. Biofeedback is a training technique that may be useful if you have problems locating the correct muscles. With biofeedback, you're connected to electrical sensors that help you to receive information (feedback) about your body (bio). This feedback helps you to focus on making subtle changes in your body, such as flexing your pelvic muscles, more successfully.
- Try a bladder-friendly diet - Avoid foods like caffeine, chocolate, alcohol, carbonated beverages and spicy foods. All of these can alter the acidity of your urine, making your incontinence symptoms worse. Avoid smoking.
- Stay hydrated - While drinking too much of anything will create an urge to go, a critical tool for dealing with incontinence is to drink plenty of water. Now, this may sound counterintuitive. After all, if you feel like you have to urinate, it might make sense to limit your fluid intake. However, not drinking enough water results in highly concentrated urine, which will irritate your bladder. Make sure that you drink 6 to 8 glasses of water a day.
- Get moving - Weight management can help to alleviate the symptoms of adult incontinence, as extra pounds put pressure on the bladder’s muscles, which can lead to stress incontinence. Simply going for more walks around the neighbourhood is an easy, straightforward way to get moving.
- Practice breathing techniques - The pelvic floor muscles, as part of the stabilising muscles of the trunk, work closely with the abdominal muscles and diaphragm, so functional improvements can be achieved through conscious breathing techniques, and the extension of the low-pressure expiratory flow leaves room for increased activation of the closure structures. Breathing techniques are helpful in optimising respiratory coordination.
- Seek advice of a specialist women’s health physiotherapist: some women struggle with overly tight pelvic floor just as much as a lax one which can result in urinary dysfunction. Get your pelvic floor checked by a specialist to find appropriate solutions. They might indicate the use of a pelvic toner which can help too.
