
We’re diving into bladder prolapse, because sometimes your bladder decides to “drop in” a little too literally. Don’t worry, we’ll make sense of it together.
Table of content:
What is the pelvic floor and prolapse?
In order to understand prolapse you need to learn about the pelvic floor. The pelvic floor is a group of muscles and connective tissues that act like a supportive hammock at the base of a woman’s pelvis. These muscles help hold the bladder, uterus and bowel in place, and they play a key role in bladder control, bowel function and sexual wellbeing. When the pelvic floor is strong, everything stays supported and works smoothly; when it weakens, for example due to childbirth, menopause, ageing or strain, you may notice issues like leaks, pressure or discomfort.
A prolapse happens when the pelvic floor muscles and supporting tissues become weakened and can no longer hold the pelvic organs, such as the bladder, uterus, or bowel, in their usual position. As a result, one or more of these organs can drop down and press into the vaginal wall, leading to symptoms.
Let’s explain some medical terms:
- Uterine prolapse – this is when the uterus slips down into the vagina
- Rectocele – where the rectum bulges into the vagina and leads to symptoms like the sensation of not fully opening your bowels, or difficulties passing stool.
- Cystocele – bladder prolapse, where the bladder bulges into the vagina.
Symptoms of bladder prolapse
- Difficulty urinating
- Feeling like you still have to ‘go’ even immediately after urination
- A dragging sensation in the vagina, or the sensation that there is extra tissue or a lump in the vagina
- Tissue protruding from the vagina
- Heaviness or pressure in the vaginal area
- Frequent urinary tract infections
- Stress incontinence: leaking a urine when sneezing, coughing, exercising or lifting heavy objects
- Painful intercourse
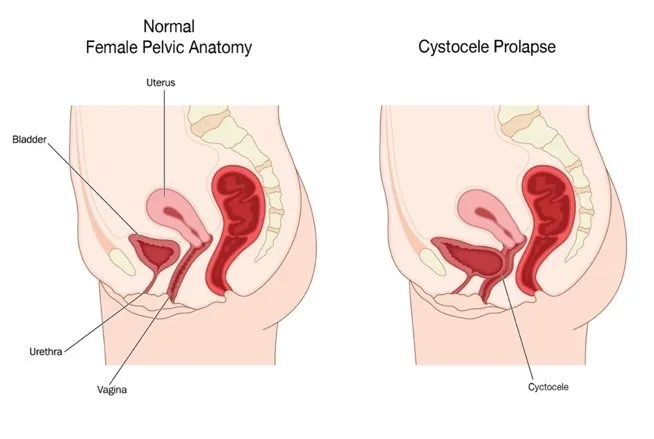
Why does bladder prolapse happen?
The pelvic floor muscles work together with the front wall of the vagina to support the bladder, a hollow organ that fills up with urine, signalling when it’s time to go. When the pelvic floor muscles surrounding the bladder weaken or loosen, the bladder is no longer supported, causing it to slouch against the vagina and creating an obstruction or bulge in the vaginal cavity.
One of the risk factors for developing bladder prolapse is menopause as the lower levels of oestrogen associated can lead to weakness in the pelvic floor and vagina. If they deteriorate enough, the bladder is no longer supported and can fall into the vagina.
Other risk factors for bladder prolapse are:
-
Pregnancy and in particular vaginal delivery
-
Surgery, such as a hysterectomy
-
Excessive strain on the pelvic floor for example from long-term constipation, lifting heavy objects, a chronic cough or weight gain
In women, the pelvic floor muscles and the connective tissues of the vagina help support the bladder and keep it in its usual position. If these muscles or tissues become weakened or stretched, the bladder can drop down (prolapse) and press into the front wall of the vagina. This can lead to a feeling of pressure, bulging, or changes in bladder control.
Menopause is one risk factor. After menopause, lower oestrogen levels can reduce the strength and elasticity of the vaginal tissues, making prolapse more likely. However, prolapse can happen at any age and usually results from a combination of factors that weaken the pelvic floor over time.
Known risk factors include:
- Pregnancy and vaginal birth – especially if labour was long, the baby was large, or instruments (forceps/ventouse) were used
- Pelvic surgery, including hysterectomy
- Long-term strain on the pelvic floor, such as ongoing constipation, frequent heavy lifting, or a chronic cough
- Being overweight, which increases pressure on the pelvic floor
- Ageing, which naturally reduces muscle strength over time
How is bladder prolapse classified?
Healthcare professionals usually describe bladder prolapse (cystocele) as mild, moderate or severe, a way of understanding the stages is based on how far the bladder has descended into or beyond the vagina:
- Stage 1 (mild): The bladder has dropped slightly, but sits well inside the vagina.
- Stage 2 (moderate): The bladder has descended to the opening of the vagina.
- Stage 3 (severe): Part of the bladder bulges outside the vaginal opening.
- Stage 4 (very severe/complete prolapse): The bladder is completely outside the vagina.
I have bladder prolapse, now what?
Well the good news is that there are lots of measures that can help!
-
Pelvic floor exercises.
Strengthening the pelvic floor is one of the most effective first-line treatments. These muscles support the bladder, uterus and bowel, and regular exercises can ease symptoms and prevent prolapse from worsening. A pelvic health physiotherapist can teach you how to do the exercises correctly. Most people need to practise daily for at least 3 months to see improvement. Pelvic floor exercise programmes are available online, including apps like the Squeezey app and many women find it helpful to build them into everyday activities like sitting at a desk or waiting for the kettle to boil.
- Lifestyle changes
Certain habits can reduce pressure on the pelvic floor. You may be advised to:
- avoid heavy lifting where possible
- treat constipation with diet changes (such as more fibre and fluids) or laxatives if recommended
- maintain a healthy weight
- manage a chronic cough (for example, due to smoking, asthma or reflux) These steps help prevent further strain on the pelvic floor and may improve symptoms.
- Vaginal oestrogen
For women after menopause, low-dose vaginal oestrogen can strengthen and improve the elasticity of the vaginal tissues, which may help reduce prolapse symptoms and make pessaries more comfortable to use. This type of oestrogen acts locally and is considered safe for most women, though it should be discussed with a doctor if you have a history of certain cancers or conditions.
- Women’s health physiotherapy and biofeedback
Specialist pelvic health physiotherapists can offer tailored pelvic floor rehabilitation, including techniques such as biofeedback, which uses sensors or visual cues to help you learn how to correctly contract and relax the pelvic floor muscles. Biofeedback can be helpful for some women with bladder prolapse, particularly in mild to moderate cases, as it supports more effective strengthening and improves awareness of pelvic floor function. Your GP can refer you to a physiotherapist with pelvic health training if this treatment is appropriate for you.
- Pessary
A pessary is a silicone device placed inside the vagina to support the bladder and vaginal walls. It can be a very effective option for many women, including those wishing to avoid surgery. A healthcare professional will fit the right type and size for you. Some pessaries can be removed and cleaned at home; others require regular checks and cleaning in clinic. They are generally safe but can occasionally cause discharge, irritation or slipping out, so follow-up appointments are important.
- Surgery
Surgery is considered when symptoms are significant or when other treatments haven’t helped. The most common operation for bladder prolapse is an anterior vaginal wall repair (anterior colporrhaphy), which tightens the tissues supporting the bladder. Vaginal mesh is no longer routinely used for prolapse surgery in the UK. Surgery can be done under general, spinal or local anaesthetic. Recovery times vary, and you will be advised to avoid heavy lifting and constipation afterwards.
- Managing leaks while seeking treatment
Some women experience urinary leaks as part of their symptoms. Absorbent pads or liners can help you stay comfortable while treatment is ongoing. Choose unscented products designed for bladder leakage rather than menstrual pads, as they absorb differently.
Bladder leaks are common, but that doesn’t mean that they are normal or that you need to put up with symptoms. If you think you may have bladder prolapse, it’s important to see your GP or a pelvic health specialist. They can confirm the diagnosis, explain your options, and help you choose the treatment that best suits your symptoms, health and lifestyle.
While you’re going through these treatments, it can be helpful to wear protection against little urine leaks resulting from your condition, so you can feel as comfortable as possible. Always Discreet liners and pads come in a variety of different sizes and absorbencies to match urinary needs. Always Discreet liners and pads quickly turn liquid and odours into gel to keep you confident and comfortable throughout your day.
* If you are going through menopause or experiencing bladder leaks, always make sure to consult your doctor or a health specialist for these medical conditions.
* Always Discreet products are not products to help with menopause, but medical devices for bladder leaks, which may be a symptom experienced by some women during menopause.





